Degenerative Disc Disease
What is degenerative disc disease?
Nearly everyone's spinal discs show signs of wear as they age. Not everyone, however, will have degenerative disc disease. Not actually a disease, this is a condition in which a damaged disc causes pain. A wide range of symptoms and severity is associated with this condition.
Spinal Discs
The discs are like shock absorbers between the bones of the spine and are designed to help the back stay flexible while resisting terrific forces in many different planes of motion. Each disc has two parts:
- A firm, tough outer layer, the anulus fibrosus. The outer portion of this layer contains nerves. If the disc tears in this area, it can become quite painful.
- A soft, jellylike core, the nucleus pulposus. This part of the disc contains proteins that can cause the tissues they touch to become swollen and tender. If these proteins leak out to the nerves of the outer layer of the disc, they can cause a great deal of pain.
Unlike other tissues of the body, the disc has very low blood supply. Once a disc is injured, it cannot repair itself, and a spiral of degeneration can set in with three stages that appear to occur over 20 to 30 years:
- Acute pain makes normal movement of the back difficult
- The bone where the injury occurred becomes relatively unstable. Over a long period of time, the patient will have back pain that comes and goes.
- The body restabilizes the injured segment of the back. The patient experiences fewer bouts of back pain.
What causes degenerative disc disease?
Several factors can cause discs to degenerate, including age. Specific factors include:
- The drying out of the disc. When we are born, the disc is about 80 percent water. As we age, the disc dries out and doesn't absorb shocks as well.
- Daily activities and sports, which cause tears in the outer core of the disc. By age 60, most people have some degree of disc degeneration. Not everyone at that age has back pain, however.
- Injuries, which can cause swelling, soreness and instability. This can result in low back pain.
What are the symptoms of degenerative disc disease?
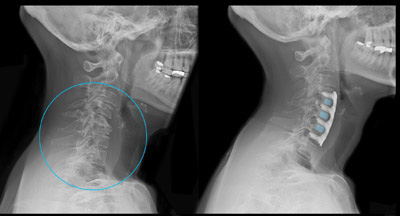
|
The typical person with degenerative disc disease is active, otherwise healthy and in his or her 30s or 40s.
Common symptoms of this condition include:
- Pain that is worse when sitting. While seated, the discs of the lower back have three times more load on them than when standing.
- Pain that gets worse when bending, lifting or twisting.
- Feeling better while walking or even running than while sitting or standing for long periods of time.
- Feeling better changing positions often or lying down.
- Periods of severe pain that come and go. These last from a few days to a few months before getting better. They can range from nagging pain to disabling pain. Pain can affect the low back, buttocks and thighs or the neck, depending on where the affected disc is, radiating to the arms and hands.
- Numbness and tingling in the extremities.
- Weakness in the leg muscles or foot drop, a possible sign of damage to the nerve root.
How is degenerative disc disease diagnosed?
A diagnosis is based on a medical history and a physical examination, as well as the symptoms and the circumstances where the pain started. Magnetic resonance imaging can show damage to discs, but it alone cannot confirm degenerative disc disease.How is degenerative disc disease treated?
Treatment options include:
- Artificial disc replacement
- Surgical intervention
- Nonoperative treatment of symptoms, including acupuncture, back braces and pain management
Key points
- Degenerative disc disease isn't actually a disease, but rather a condition in which a damaged disc causes pain. This pain can range from nagging to disabling.
- The condition can be caused by the drying out of the disc over time, daily activities, sports and injuries.
- Treatment options include disc replacement, other surgical interventions, and nonsurgical options such as acupuncture, back graces and pain management.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
- Know the reason for your visit and what you want to happen.
- Before your visit, write down questions you want answered.
- Bring someone with you to help you ask questions and remember what your provider tells you.
- At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
- Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are.
- Ask if your condition can be treated in other ways.
- Know why a test or procedure is recommended and what the results could mean.
- Know what to expect if you do not take the medicine or have the test or procedure.
- If you have a follow-up appointment, write down the date, time, and purpose for that visit.
- Know how you can contact your provider if you have questions.
Cedars-Sinai has a range of comprehensive treatment options.
Get the care you need from world-class medical providers working with advanced technology.